Delivering innovative program solutions that result in improved health outcomes
Collaborating to achieve the promises of healthcare reform
Maximus possesses unmatched experience with the Affordable Care Act (ACA), as our support covers all the various facets of the law, ranging from choice counseling and eligibility appeals to education and outreach, training, and value-based programs. Through our work managing citizen engagement centers for publicly funded healthcare recipients, we answer thousands of ACA-related questions every day, helping consumers with gaining access to health insurance.
Learn how our contact centers connect millions of citizens to government
Medicare appeals
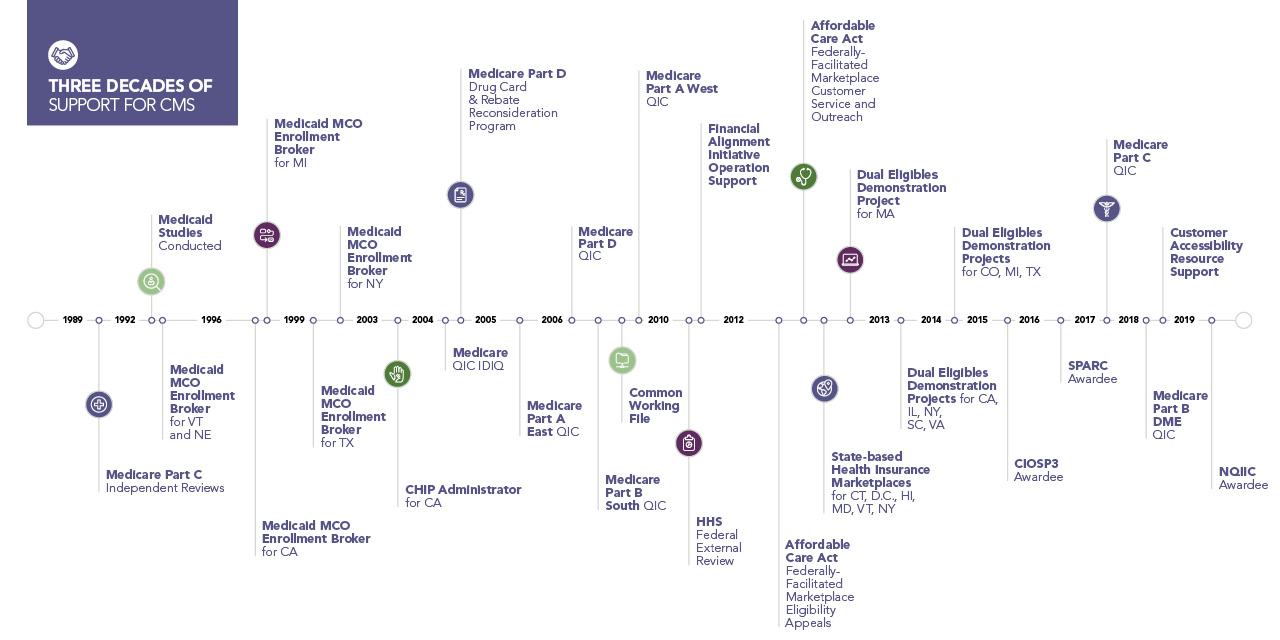
Since 1989, CMS has relied on Maximus to provide Medicare beneficiaries and providers with independent, conflict-free appeal decisions of health insurance denials. Because we have no financial affiliation with insurers or providers, we are the only conflict-free Independent Review Organization (IRO) providing Medicare appeals. We receive and review more than 600,000 appeals claims a year for Medicare, helping expedite the process to appeals determinations for citizens.

Streamlining independent medical review process for digital transformation
As a federal agency within the United States Department of Health and Human Services (HHS), the Centers for Medicare & Medicaid Services (CMS) is dedicated to advancing health equity, expanding coverage, and improving health outcomes for the American public.
By using quality processes and technologies that streamlines the most complex QIC operations programs, Maximus was able to increase efficiency and improve its appeal process quality at scale. As a trusted technology and solutions service partner of CMS, we are proud to support the advancement of the nation’s critical health needs, transform clinical care, and establish a blueprint for the future of public health.
Learn more about our work with the CMS QIC
Connecting citizens with access to health information
Maximus supports the CMS Customer Accessibility Resource Staff in its effort to enhance beneficiary services and access to health information. This work is critical to achieving CMS’ mission to improve communications and implementations of agency enterprise solutions to meet the requirements of Section 504 of the Rehabilitation Act of 1973. As health communication experts, we specialize in making health information accessible and easy to understand.
Discover how our Center for Health Literacy empowers citizens to make decisions
Improving health outcomes at CMS
The Centers for Medicare & Medicaid Services, CMS, provides health coverage to more than 100 million people through Medicare, Medicaid, the Children’s Health Insurance Program, and the Health Insurance Marketplace.
Through a strategic collaboration with the CMS, Maximus delivered support for all functions in the operation of the appeals process associated with the federal and state-bases exchanges under the Affordable Care Act including both operations and digital tasks. As a trusted technology and service solutions partner, Maximus is proud to support the advancement and elevation of the nation’s public health.
Learn more about our work with the CMS